Eduardo Alguacil, MRCVS Uplands Way Veterinary Practices
The liver is the largest organ in the body of the horse. It is in charge of metabolising carbohydrates, proteins, and fat and can also excrete numerous toxic compounds. It can perform different functions, including endocrine (secretes hormones/products directly into the blood) and exocrine (secretes hormones/products through a duct) functions. Most of the nutrients absorbed from the gastrointestinal tract pass via portal circulation straight to the liver, where they are metabolised. They are then repackaged, stored, or exported to peripheral tissues. Humans and horses can survive with a liver that is not 100% healthy as this organ can regenerate itself, so it provides protection against permanent damage. Horses might survive with only 20% of a functioning liver, although when the damage is more than 80%, they can start to develop clinical signs (Durham et al., 2003).
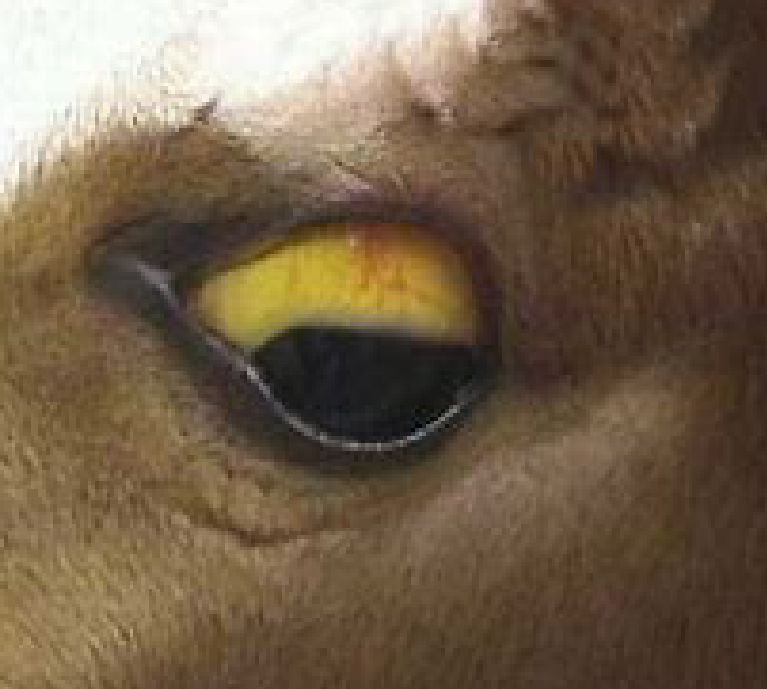
Figure 1. Yellowing of the mucus membranes indicates jaundice, a symptom of liver damage.
The liver in the horse is susceptible to developing disease as it works as a clearance organ for many toxins, and grazing animals like horses are more predisposed to develop liver disease (West,1996). The only way to identify liver disease is with the clinical signs, as the liver cannot be seen, heard, or palpated. When they start to show clinical signs, the damage could be irreversible. Early clinical signs could be unspecific such as weight loss, anorexia, lethargy, abdominal pain (colic) and jaundice (Figure 1). Other clinical signs could be stridor (abnormal respiratory noise), photosensitisation (skin changes due to ultraviolet sunlight) or diarrhoea. In severe or advanced cases, the horse can develop hepatic encephalopathy (developing neurologic problems). When the horse develops icterus (yellowing of the skin, gums, and whites of the eyes) this is due to the liver's incapacity to take up, conjugate and excrete bilirubin. Before this happens, we have some laboratory tests that may detect disease before the failure. In these tests, we can see how some functions of the liver fail, giving a prognosis and a progression of the clinical signs (Parraga et al., 1995). Routine biochemical tests, including hepatic enzymes such as gamma-glutamyl transferase (GGT), glutamate dehydrogenase (GLDH), alkaline phosphatase (ALP) and aspartate aminotransferase (AST), can tell us if liver disease is present. However, to assess liver function more accurately we need a more specific test to measure specific liver parameters such as bile acid and bilirubin concentrations. An additional blood test can give extra information like prolonged blood clotting times, hyperglobulinaemia and increased ammonia concentration, however the most accurate test for the diagnosis of liver disease is a liver biopsy. Taking a sample from the organ lets us know the causes and the severity of the liver disease. Other tests we can carry out are a hepatic ultrasound to check the hepatic size, the appearance of the liver, look for tumours or abscesses, and abdominal radiographics with contrast to determine if the liver presents any obstruction.
MAIN LIVER DISEASES:
TOXICS
Pyrrolizidine alkaloid (PA) poisoning: PA toxicity is commonly due to ingestion of Common Ragwort in the UK (Figure 2), but other plants also contain this toxin (Clarke et al., 1981; Caloni & Cortinovis, 2015). When the PA are ingested, the alkaloids are broken down to pyrrols in the liver. Although unpalatable, ragwort consumption occurs when poor pasture or hay grazing is contaminated (Vandenbroucke et al., 2010). Most horses with PA poisoning develop chronic and delayed clinical signs. The main clinical signs are weight loss, icterus and lethargy although horses and ponies may not become unwell until a year after ingestion of PAs, making such toxicity challenging to diagnose. The liver enzymes are altered before showing any other clinical signs. The serum GGT, ALP and total bile acids concentrations are the most sensitive indicators of this chronic disease. The animal starts to deteriorate, developing other symptoms such as respiratory disease due to bilateral laryngeal paralysis (Fu et al., 2002; Lahse et al., 2018). Although the origin of this paralysis is unknown, it could be related with hyperammonaemia as it can develop functional neuromuscular disorders (McGorum et al., 1999). Most cases cannot be treated once the clinical signs have started, especially when we have found histopathological changes, the liver enzymes are altered, and the animal presents neurological signs. In early stages, before the horse suffers changes in the liver, removing the feed containing PAs, and supporting liver function, the horse might survive. Mycotoxins: These are naturally occurring toxic substances which are produced by moulds and fungi in your horse’s forage (Penicillium and Aspergillus) or pasture (Fusarium and Endophyte toxins). The environmental conditions can lead to an increase in the levels of toxins produced, with toxins able to be stored on the grass or forage for a long time. There are a variety of clinical signs, such as liver disease, colic, hypersensitivity, abortions, and neurological disorders.

Figure 2. Ragwort (Senecio jacobaea) is a common cause of liver damage in horses.
Other Hepatotoxins: Many products can be toxic to the liver, including other plants, chemicals and drugs administered by your veterinarians. Indeed, clinical signs and laboratory tests do not differentiate between the different toxins, but with the diagnosis of liver disease and a good anamnesis the clinician can try to identify the specific toxin.
ACUTE HEPATITIS (THEILER’S DISEASE)
Acute hepatitis is developed suddenly in a short term, producing inflammation of the liver. The causes of this disease are diverse, such as administration of tetanus antitoxin, infection (blood transfusions), poisons or undefined causes (Hjerpe, 1964). Most of the cases are developed in the summer season, and it may be that a vector (intermediate carrier or transporter) is related as some horses present acute hepatitis that have not been administered any serum product but are exposed to horses which have. Lactating mares that receive tetanus antitoxin at foaling seem to be more susceptible. The clinical signs appear between 4-10 weeks after exposure. Acute hepatitis can be sporadic, but in most cases, there are more animals involved. The clinical signs are lethargy, icterus, and anorexia. The urine has a dark colour because of the high bilirubin concentration. Weight loss is not common as the signs are acute. Severe cases can develop hepatic encephalopathy. Death may occur suddenly in 50% to 60% (with an overall death rate as high as 88%) of affected horses. For diagnosis, it is necessary to perform a liver biopsy to confirm, although, with the history, clinical signs and blood tests we can make an approach to the diagnosis. There is no specific treatment for acute hepatitis, but your veterinarian can give some supportive therapy.
CHOLANGIOHEPATITIS
Cholangiohepatitis is severe inflammation of the bile ductus and adjacent liver, and it can lead occasionally to liver failure in horses. This disease appears as a consequence of an intestinal infection migrating to the liver (most of the cases by Salmonella spp.) or parasite infection such as flukes (Figure 3). It has also been associated with stones in the bile duct, intestinal inflammation, tumours and some toxins.
_1000.jpeg)
Figure 3. Grazing horses with sheep can lead to liver fluke infection.
The clinical signs could be more related with colon damage, but liver enzymes are increased, and bilirubin and total bile acid concentrations may be disproportionately high. For diagnosis we can evaluate with ultrasound the length of the ductus, checking if it is larger than normal, and then a liver biopsy is necessary to obtain a sample of tissue to perform a culture. For the treatment, we can use antibiotics as they are excreted in the bile.
CHRONIC ACTIVE HEPATITIS
This disease is a chronic inflammation in the liver. It is well described in humans and dogs. The inflammation is localised in the periportal area (Carlson & Vivrette, 1989). The aetiology is unknown, and multiple agents may be involved. The clinical signs are multiple and not specific. Most of them are related with chronic liver diseases such as depression, weight loss, and neurological signs. Fever could appear if a bacterial infection is the cause of the disease, and icterus could be present, but it is not mandatory. Some horses have moist exfoliative dermatitis at the coronary bands due to vasculitis. It is difficult clinically to differentiate these horses from those with PA toxicity. For a diagnosis, a liver biopsy is necessary and should demonstrate ongoing but chronic hepatitis. Many horses with chronic active hepatitis that is detected early before bridging fibrosis occurs can be saved. We need to make an accurate diagnosis to provide appropriate treatment, as in cases where the main cause of the disease is bacterial infection, antibiotics should be used, but when it is just related with inflammation, corticosteroids can be used.
HYPERTRIGLYCERIDAEMIA, HEPATIC LIPIDOSIS
Hypertriglyceridemia is defined as an increase in plasma triglyceride concentration, without the animal presenting associated clinical symptoms (Dunkel & McKenzie, 2003). It usually occurs as a complication more frequently in ill animals or those with high energy demands (pregnant or lactating mares), in sick animals with secondary insulin resistance, for example, a systemic inflammatory response syndrome (SIRS), in animals that cannot ingest food (chewing problems, dysphagia, prolonged fasting) or in genetically predisposed sick animals such as ponies and donkeys. In these cases, it may be primary. The most characteristic clinical signs are apathy, anorexia, depression, weight loss, hyperthermia and in more severe cases, can lead to fatty infiltration of the liver and liver failure (Mackenzie, 2011). Diagnosis is based on finding white-to-yellow opacity of the serum caused by the high lipid content. Cholesterol is also increased, indicating an increase in lipoprotein. Treatment to control hypertriglyceridaemia focuses on reversing the catabolic state in which the animal is in to stop the mobilisation of triglycerides from adipose tissue.
TREATMENT OF LIVER DISEASE IN THE HORSE
The success of treatment in liver disease is better when the disease is in the early stages or acute phases. As the liver has a good capacity to regenerate when we treat it in early stages, the outcome is usually good. The first aim of the treatment has to be to eliminate the main cause. Sometimes when it is in advanced phases, only eliminating the main cause is not enough to recover the liver function completely. When the veterinarian is going to use any drugs, they need to think about where the drug is metabolised, as it can affect the liver function. One of the most important points in the treatment of liver disease is diet management. It is essential to control the calorie intake. Feeds with readily digestible carbohydrates may help keep the blood glucose levels up. The proteins should be limited, but need to be of high quality, so the amino acids are not used for energy which increases the amount of ammonia produced. Excess protein may lead to hyperammonemia and hepatic encephalopathy, but some protein is needed for regeneration of the liver and to produce lipoprotein to mobilise fat from the liver. Diets with a high amount of amino acids could improve the grade of hepatic encephalopathy. Prevention of liver disease is the most important treatment. Reducing exposure of the animal to hepatotoxic plants, herbicide sprays, removing the horse from pastures with sheep, or using biological control such as the cinnabar moth, is the best therapy to avoid equine liver disease.
For any advice or questions you may have, please don't hesitate to reach out to our expert nutrition team. You can call 0800 585525 Monday-Friday 8:30am-5:00pm. Email [email protected], or send us a DM on social media.
REFERENCES
Caloni, F., & Cortinovis, C. (2015). Plants poisonous to horses in Europe! Equine Veterinary Education, 27(5): 269-274. Carlson, G.P., & Vivrette, S. (1989). Chronic active hepatitis in horses. In: Proceedings of the American College of Veterinary Internal Medicine Forum 7: 595.
Clarke, M., Harvey, D., & Humphreys, D. (1981). Veterinary Toxicology, 2nd ed., Bailliere Tindall: London: 203-206. Dunkel, B., & McKenzie, H.C. (2003). Severe hypertiglyceridaemia in clinically ill horses: diagnosis, treatment and outcome. Equine Veterinary Journal, 35(6): 590-595.
Durham, A. E., Smith, K. C., Newton, J. R., Hillyer, M. H., Hillyer, L. L., Smith, M. R., & Marr, C. M. (2003). Development and application of a scoring system for prognostic evaluation of equine liver biopsies. Equine Veterinary Journal, 35(6): 534–540.
Fu, P., Xia, Q., Lin, G., & Chou, M. (2002). Genotoxic pyrrolizidine alkaloids - mechanisms leading to DNA addict formation and tumorigenicity. International Journal of Molecular Sciences, 3: 948-964. Mackenzie, H,C. (2011). Equine Hyperlipidemias. Veterinary Clinics of North America: Equine Practice, 27: 59-72.
Hjerpe, C.A. (1964). Serum hepatitis in the horse. Journal of American Veterinary Medical Association, 144: 734-74. Lahse, J., Paredes, E., Gonzalez, C., Koene, M., & Mageed, M. (2018). Pyrrolizidine alkaloid toxicosis and hepatic encephalopathy in horses in Easter Island, Chile. Australian Journal of Veterinary Science, 50:107-110.
McGorum, B., Murphy, D., Love, S., & Milne, E. (1999). Clinicopathological features of equine primary hepatic disease: a review of 50 cases. Veterinary Record, 145: 134-139.
Parraga, M.E., Carlson, G.P., & Thurmond, M. (1995). Serum protein concentrations in horses with severe liver disease: a retrospective study and review of the literature. Journal of Veterinary Internal Medicine, 9: 154-161.
Tennant, B. (1978). Acute hepatitis in horses: problems of differentiating toxic and infectious causes in the adult. Proceedings of the American Association of Equine Practitioners, 24: 465-471.
Vandenbroucke, V., Van Pelt, H., De Backer, P., & Croubels, S. (2010). Animal poisonings in Belgium: a review of the past decade. Vlaams Diergeneeskundig Tijdschrift, 79: 259-268.
West, H. J. (1996). Clinical and pathological studies in horses with hepatic disease. Equine Veterinary Journal, 28: 146–156.


_800.jpeg)